Treatment for Your Child’s Aortic Stenosis (AS)
Your child has aortic stenosis (AS). This condition occurs when the aortic valve doesn’t open all the way. It can also occur when the area above or below the valve is too narrow. As a result, blood flow from the left ventricle to the rest of the body (except the lungs) is blocked. Children with severe or critical AS need treatment right away. Treatment choices include balloon valvuloplasty, aortic valve repair, and aortic valve replacement.
Your child’s experience with balloon valvuloplasty
Balloon valvuloplasty is a heart procedure using a thin, flexible tube called a catheter. A cardiologist who has special training to use these catheters to treat heart problems (cardiac catheterization) does this procedure. It lasts about 2 to 4 hours and takes place in a catheterization lab at the hospital. You’ll stay in the waiting room during the procedure.
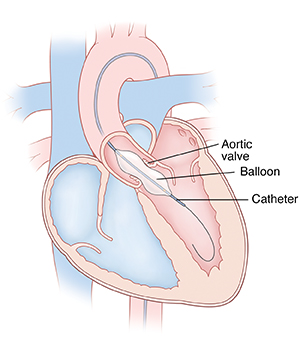 |
| A balloon on a catheter is inflated to open the stenotic (narrowed) aortic valve. |
-
Before the procedure. You’ll be told to keep your child from eating or drinking anything for a certain amount of time before the procedure. Follow these instructions carefully.
-
During the procedure. The health care provider inflates a balloon on the tip of the catheter to open the stenotic (narrowed) aortic valve. Your child is given medicine (sedative or anesthesia). This is to help them relax and not feel discomfort or pain during the procedure. A breathing tube may be placed in your child’s trachea (windpipe) during this time. Special equipment monitors your child’s heart rate, blood pressure, and oxygen levels. The catheter insertion site (the groin) is cleaned and numbed. Then the catheter is inserted into a blood vessel in the groin. With the help of live X-rays, the catheter is guided up through this blood vessel into the heart. The provider may inject contrast dye through the catheter. The dye allows the inside of the heart to be seen on X-rays. The provider will inflate a small balloon at the end of the catheter one or more times within the aortic valve. This forces the valve leaflets to open. Then the catheter and balloon will be removed.
-
After the procedure. Your child is taken to a recovery room. You can stay with your child during much of this time. It may take several hours for medicines to wear off. Pressure is applied to the catheter insertion site to limit bleeding. The provider will tell you how long your child needs to lie down and keep the insertion site still. Your child is cared for and monitored until they can leave the hospital. An overnight hospital stay is often needed.
Risks and complications of balloon valvuloplasty
The risks and complications include:
-
A reaction to the contrast dye.
-
A reaction to the sedative or anesthesia.
-
Pain, swelling, redness, bleeding, or drainage at the catheter insertion site.
-
Leakage of blood through the aortic valve back into the left ventricle (valve insufficiency).
-
An abnormal heart rhythm (arrhythmia).
-
The need for further treatment to repair or replace the valve.
-
Injury to the heart or a blood vessel.
-
Death.
Your child’s experience with valve repair or replacement
Valve repair or replacement is done with open heart surgery. A pediatric heart surgeon does the heart surgery. The surgery lasts about 4 to 6 hours. It takes place in an operating room in a hospital. You’ll stay in the waiting room during your child’s surgery.
-
Before surgery. You’ll be told to keep your child from eating or drinking anything for a certain amount of time before surgery. Follow these instructions carefully.
-
During surgery. Your child is given medicine (sedative and anesthesia) to sleep and not feel pain during surgery. A breathing tube is placed in your child’s trachea (windpipe) during this time. Special equipment monitors your child’s heart rate, blood pressure, and oxygen levels. Your child is also placed on a heart-lung bypass machine. This allows blood to keep flowing to the body while the heart is stopped so that it can be operated on. The surgeon will make an incision in the chest through the sternum (breastbone) to get to the heart.
-
With valve repair, the surgeon opens the aortic valve by cutting through thickened or fused leaflet tissue. A patch can also be used to make the valve larger, if needed.
-
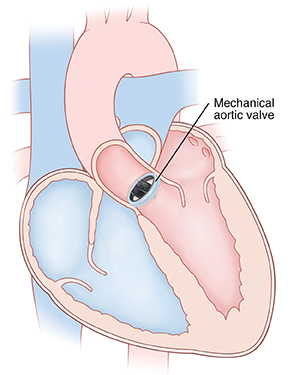
With valve replacement, the surgeon replaces the aortic valve with an artificial one that is either biological or mechanical. Biological valves are made from human or animal tissue. Mechanical valves are made from material such as ceramic or metal. Or the child's own pulmonary valve may be removed and used to replace the aortic valve. This is known as the Ross procedure It can be especially helpful as the valve grows with your child. The pulmonary valve is then replaced with a valve from a human donor (homograft).
-
After surgery. Your child is taken to a critical care unit to be cared for and monitored. You can stay with your child during much of this time. They will stay in the hospital for at least 5 to 7 days. When your child is ready to leave the hospital, you’ll be given instructions for home care and follow-up.
Risks and complications of heart surgery
Risks and complications may include:
-
A reaction to the sedative or anesthesia.
-
Leakage of blood through the aortic valve back into the left ventricle (valve insufficiency).
-
An abnormal heart rhythm (arrhythmia).
-
An infection.
-
Bleeding.
-
Nervous system problems, such as a seizure or stroke.
-
An abnormal buildup of fluid around the heart and lungs.
-
Death.
When to call the doctor
After the balloon valvuloplasty procedure or heart surgery, call 911 right away if your child:
After the balloon valvuloplasty procedure or heart surgery, call your child's health care provider right away if your child has:
-
Increased pain, swelling, redness, bleeding, or drainage of an incision or insertion site.
-
A fever. Ask the provider about target temperatures for your child.
-
Increased tiredness.
-
Prolonged nausea or vomiting.
-
A cough that won’t go away.
Online Medical Reviewer:
Dan Brennan MD
Online Medical Reviewer:
Scott Aydin MD
Online Medical Reviewer:
Stacey Wojcik MBA BSN RN
Date Last Reviewed:
2/1/2025
© 2000-2025 The StayWell Company, LLC. All rights reserved. This information is not intended as a substitute for professional medical care. Always follow your healthcare professional's instructions.